MSU Care Services Eligibility
Eligibility Criteria
MSU Care provides primary care services and prescription medication to qualified adults
between the
ages of 18 and 64 years old.
Qualified adults are those without health insurance or covered by Medicaid, Managed
Medicaid, and
Dual Enrolled Medicaid/ Medicare.
Uninsured adults will receive services provided by MSU Care free of charge during
their eligibility
period.
Uninsured Adults must also meet income guidelines. Household, or family income, needs
to equal or
be less than 200% of the Federal Poverty Level
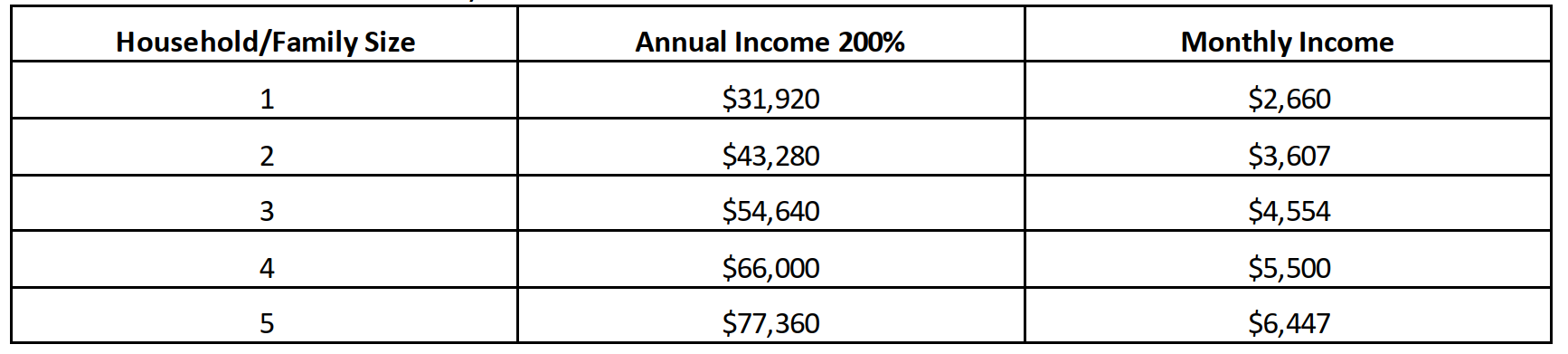
Uninsured Adults may be asked to bring the items listed below to the Clinic to complete your enrollment packet:
- Two months of the most recent pay stubs for everyone in the household
- Most current year’s federal income tax return for everyone in the household. (If taxes were not filed, MSU Care has a form to fill out.)
- Provide documentation of eligibility of federal, state, or other income benefit assistance including, but not limited to, SSI, SSD, VA, and/or Worker’s Compensation for everyone in the household.
- Applicants may be asked to provide a recent Medicaid denial letter (for uninsured adults only), verification of shelter, a signed letter of support, and/or letter of health insurance termination.
- Additional items may be required
MSU Care will not be able to schedule an appointment until all required items are received and enrollment packet is filled out
MSU Care free service eligibility is in effect for 6 months, unless you obtain Medicaid (MO Healthnet), Medicare, or any other health coverage.
We are open Mondays, Tuesdays, Wednesdays, and Fridays 8 am-12 pm and 1 pm-5 pm and
Thursdays 10 am- 1 pm and 2 pm-7 pm. The lobby is closed for lunch and the clinic is closed on weekends.
If you have questions regarding the enrollment process, please call us at (417) 837-2270 and a member of our team would be more than happy to assist you.
Patient Responsibilities
- Provide accurate, true and complete information about financial status and health coverage.
- Report any changes to financial or insurance status.
- Update eligibility information at a minimum of every 180 days.
- Keep appointments and be compliant with the treatment plan.